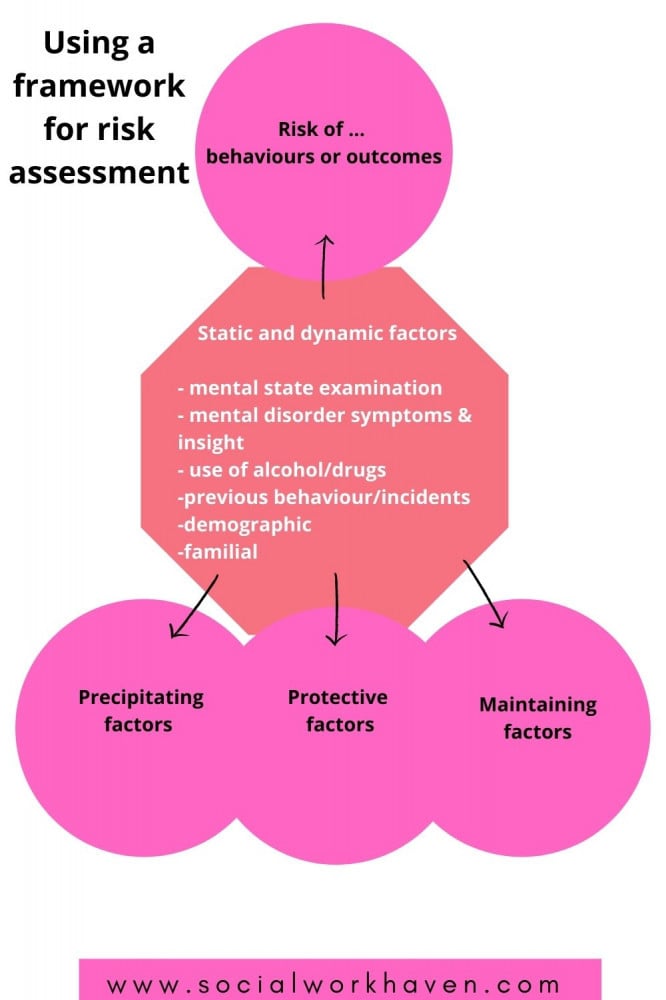
When assessing and managing risk in mental health, it is useful to consider the use of specific care frameworks or risk assessment and management models.
What is risk assessment and management in mental health?
Risk assessment and management in mental health entails people working in mental health services to have a duty of care towards the person they are supporting where their wellbeing is balanced against issues of personal and public safety.
In this example, I will use a practical and relevant tool for developing a meaningful assessment for a person who self-harms deliberately using a made up case scenario.
Case scenario
Sarah is a 45-year-old White British Woman who had an Acquired Brian Injury (ABI) following a road traffic accident 10 years ago. Sarah lives alone after her partner of 10 years passed away following a stroke.Sarah lost her job shortly afterwards.
These recent events placed a significant strain on Sarah’s relationship with her mother and financial circumstances.Sarah’s mother was concerned about her mood as she was feeling sad. Not sleeping at night was overweight and most significantly,
Sarah was losing her ability to cook for her family as she could not remember her recipe’s. Sarah had neglected her personal care and had not showered or brushed her teeth for weeks.
As Sarah’s symptoms were present for over two weeks, her mother arranged a GP appointment.
Sarah was willing to engage with health professionals to make her feel better. The GP diagnosed Sarah with depression and prescribed some anti-depressants. Sarah was later found unconscious after taking 40 tablets of antidepressants. She was subsequently admitted into hospital.
How to carry out risk assessments
Using a framework, risk assessment will require consideration of key risk issues, static and dynamic factors, risks of behaviours, triggers or precipitating factors, protective factors and maintaining factors.
With regard to Sarah, consideration was given risk to self as well as to others. It was established that the risk of presenting issues to Sarah was high and without support, her mental wellbeing could deteriorate further.
Sarah has a history of deliberate self-harm. However, she was not at risk to others as she was not violent. Protective factors identified was the fact that she had a supportive family network. In addition, Sarah’s willingness to improve her situation was also a positive indicator.
Due to Sarah’s distress, I considered the environment most suitable to assess her in. Barker (2004) highlights that during assessments, consideration should be given to time, place as well as the environmental conditions of the setting. In mental health practice, the assessment environment is key in effective assessments and promotes patient engagement during assessments.
Seeking the patient’s approval in selecting an appropriate environment also promotes person centred practice. Within this context, I asked Sarah where she would prefer to have the assessment. She opted to have it in her room in the hospital as she felt more comfortable and at ease.
When assessing Sarah, I knew it was important for me to establish a good working relationship with her by developing rapport.

Rapport according to Kensit (2000) is defined as the close relationship between people or groups and the extent to which they understand each other and communicate effectively. I felt it was important for me to build rapport with Sarah to foster her engagement in the assessment process.
According to Barker (2004), building rapport with patients fosters feelings of confidence, safety and security while, at the same time, lessening anxiety and tension.
I realise that the relationship between the patient and the professional has the potential to be very imbalanced in terms of power that we have as professionals and the power that the patient may easily feel they do not have. As a result, it was important for me to engage with Sarah in a manner that can enhance a collaborative working relationship.
Service users may have some expectations of a professional or social worker before they meet them, or may have a preexisting opinion based on their own experiences or those of others. With this in mind, I ensured that I was dressed appropriately and had familiarised myself with Sarah’s situation by reading her medical notes before meeting with her.
Trevithick (2012) also states that “engaging skills entails being explicit about what we are doing and why” (p.187). Within this context, I explained my role to Sarah and explained why I was involved in her recovery plan.
For instance, I informed Sarah that I was going to ask her some questions to find out what she struggles with and what she needs help with. I added that we will then agree on a plan that will ensure that will outline her desired outcomes and measure her progress.
Sarah’s risk status was summarised as very low (no ideas to harm self or others). I arrived at this judgement based on history of risk, recency of risk behaviour, seriousness of risk behaviour, frequency of risk behaviour, any actual or emerging patter to risk behaviour, obvious risk factors, ideation, intent, protective factors and planning.
A personalised care plan was put in place with care interventions which aimed at managing identified risks and addressing associated risk factors. I also put a contingency or crisis plan in place (reference: the dynamic CARE framework for Managing Deliberate Self-harm (DSH).
References
Barker (2004). Assessment in psychiatric and mental health nursing: in search of the whole person (2nd ed.). Cheltenham: Nelson Thrones.
Butler J (2014) Assessing Risk in Community Mental Health Services
Butler J & Lees G (2000) Assessing and Managing Risk in People with Severe Mental Illness.
Jacob K. S. (2015). Recovery model of mental illness: a complementary approach to psychiatric care. Indian journal of psychological medicine, 37(2), 117-9.
Jaffe, M. (2018). Wellness and Recovery Action Plan. http://mentalhealthrecovery.com/ Retrieved on 31st December 2018.
Jahn H. (2013). Memory loss in Alzheimer’s disease. Dialogues in clinical neuroscience, 15(4), 445-54.
Johnson, R. & Wiggs, P. (2011). ‘Change management–or change leadership?’, Journal of Change Management. 3 (4). pp.311-17. doi: 10.1155/2011/352627
Kensit, D. A. (2000). Rogerian theory: A critique of the effectiveness of pure client-centred therapy, Counselling Psychology Quarterly, 13:4, 345-351, DOI: 10.1080/713658499
Stobbe, E. (2006). Social isolation and mental illness. http://brainblogger.com/2006/05/15/anti-stigmatization-social-isolation-and-mental-illness/ Retrieved on 30th of December 2018.
The International Disease Manual (2018). Retrieved from https://www.who.int/classifications/icd/en/ Accessed on 21st December 2018.
Wilson, K, Ruch, G, Lymbery, M & Cooper, A (2011) Social Work: An Introduction to Contemporary Practice, Harlow: Longman
World Health Organisation (2017). Global Health Observatory date. https://www.who.int/gho/publications/world_health_statistics/2017/en/ Accessed on 6th December 2018.
Wrycraft, N. (2015). Assessment and Care Planning in Mental Health Nursing. Maidenhead: Open University Press.
Xie, H. (2013). Strengths-based approach for mental health recovery. Iranian journal of psychiatry and behavioral sciences, 7(2), 5-10.